April 11th, 2023
How to Increase Enrollment: 17 Ways Research Sites Can Improve Clinical Trial Workflows
By OneStudyTeam

We have seen clinical research sites accelerate their patient enrollment timeline by four weeks. We have also seen sites enroll 41% more patients in a clinical trial than industry average.
So – How can sites improve their enrollment workflows? How can sites work to increase enrollment? It's not a secret. Sites that improve enrollment performance take strategic and proactive steps to make it happen. By improving their workflows, they can increase their enrollment numbers.
Ready to do the same? Start with these 17 straightforward tips toward clinical trial workflow optimization at your site.

(1) Digitize your patient database
(2) Digitally pre-screen every patient
(3) Rescreen patients if applicable
(4) Connect with sponsor recruitment partners
(5) Follow up with patient referrals quickly
(6) Follow up with patient referrals multiple times
(7) Categorize patients by enrollment statuses
(8) Track recruitment sources
(9) Track diversity data
(10) Sync team calendars
(11) Digitize patient visit checklists
(12) Send visit reminders to patients
(13) Set up visit reminders for site staff
(14) Take the time to fully educate patients about the trial
(15) Discuss the possible benefits of trial participation with patients
(16) Set up automated processes around clinical trial billing.
(17) Notify sponsors of obvious obstacles early
1. Digitize your patient database for ease of updates and trial assignments.
It’s not uncommon for site teams to be working within different portals to connect with each sponsor across trials. On top of that, spreadsheets and paper logs are traditionally part of the mix. Simplify your workflow by consolidating patient information into one digital database for daily use across clinical trials. This can:
- Allow quick communication of updates and next steps through patient notes
- Enable you to filter patients based on I/E criteria and diagnoses to match them to the right trial faster.
- Reduce redundant or time-consuming communication.
- Empower you to update and store data with greater accuracy.
2. Digitally pre-screen every patient to build out your database of candidates across trials.
While pre-screening for your clinical trials takes time at the beginning of enrollment, it saves time during the enrollment period and prevents eligible patients from falling through the cracks. In addition, pre-screening for one trial can help you easily find patients that may be eligible for another trial. To get the most out of your pre-screening work:
- Base questions off of I/E criteria.
- Conduct questionnaires online or by phone to avoid extra visits.
Robust pre-screening practices ensure the most eligible patients move to the screening phase, helping to reduce possible screen failures. Keep in mind: After pre-screening, 52.9% of candidates who reach their screening visit are likely to progress to enrollment.
3. Rescreen patients if applicable, to maximize candidates who have already expressed interest in trial participation.
You will already know from reading the protocol whether sponsors are allowing certain patients to be rescreened. Maybe a patient with a certain medication in their system could pass screening if they have a week longer in their washout period. Maybe a patient with insufficient glucose levels could pass screening the next day after fasting correctly. Whatever the reason, rescreening can maximize the enrollment of:
- Patients who have already met all other pre-screening criteria.
- Patients who have already signed informed consent forms to participate in the trial.
- Patients from a limited pool of candidates, such as those being considered for a rare disease clinical trial.
4. Connect with sponsor recruitment partners to quickly gain more eligible patient candidates.
Having trouble finding enough eligible candidates? Good news: Many sponsors invest heavily in central recruitment tactics, including working with patient referral partners to help fill the recruitment funnel. Reach out to your sponsor to find out if they are running a referral campaign for your trial. If so:
- Opt in to get connected to patient candidates that are coming from recruitment partners or trial websites.
- See if your sponsor invests in a referral partner integration, which allows those candidates to be automatically added to your existing enrollment management platform through the referral program. This can save valuable time by preventing manual patient uploads.
5. Follow up with patient referrals quickly to prevent missed opportunities.
Don’t let patient referrals sit for long – follow up with these candidates to start pre-screening while interest in participating in the trial is still high.
- Make a point to review and contact each referred patient within 48 hours of receiving their information.
6. Follow up with patient referrals multiple times, in multiple formats, to avoid the dropoff of an interested patient.
Why spend time looking for net new patients if you already have a list of referred patients who have expressed interest in trial participation?
- Consider reaching out to each patient at least three times, ideally at different hours of the day. See if you can connect with that person at the most convenient time for them.
- Consider reaching out in two formats if necessary. Example: Send a text message and send an email. This can help maximize your chances of them replying to your message in the format that is most comfortable for them.
7. Categorize patients by enrollment status for easy visibility across your team.
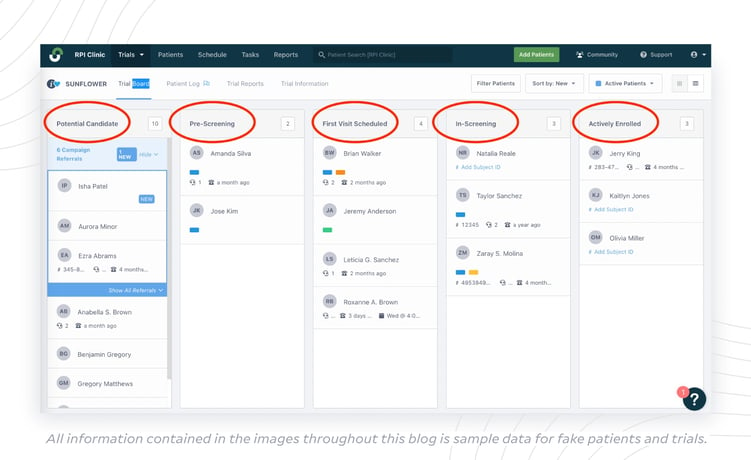
Now that you have already implemented a digital patient database (per tip 1), organize that database to help your team determine priorities while keeping an eye on the overarching view of the trial. Start with the enrollment phase. Break patients into five buckets:
- Potential Candidates
- Pre-Screening
- First Visit Scheduled
- In-Screening
- Actively Enrolled
This can help your team get focused with tasks: is there a backlog of candidates in pre-screening that your team can batch and move along to First Visit Scheduled? Is the list of Potential Candidates concerningly low, and can you address that with the sponsor to find out if a referral campaign is an option?
Here is an example from our patient enrollment management platform, StudyTeam:
8. Track recruitment sources to prioritize the ones that work.
Save time with patient recruitment by gaining visibility into which sources – social media posts, social media ads, recruitment vendors, etc. – bring in the most eligible patients. To track recruitment source data, just add the recruitment source for each patient into your patient profiles as part of your regular patient management and pre-screening process. This can help you:
- Identify which recruitment sources are actually bringing in patients – and the most eligible patients – for the trial.
- Determine which sources are not bringing in enough patients.
- Prioritize managing and budgeting for the sources that perform the best.
Bonus: When sites share these insights with sponsors, sponsors can make informed decisions about prioritizing additional recruitment resources, like clinical trial websites.
9. Track diversity data to ensure the right populations are being recruited.
Ensure your trials are accessible for every patient, including communities traditionally underrepresented in research. To track diversity data, simply input race and ethnicity data for each patient into your patient profiles as part of your regular patient management and pre-screening process. When you do this:
- You will be able to track the demographics of a trial earlier, making it easy to share any findings with your sponsor.
- You will be able to take action as needed, such as following up with certain demographic groups to recruit a more representative patient population.
- You will have clear insight into whether you are on track to help your sponsor meet their diversity goals for enrollment.
Race and ethnicity data reporting between sites and sponsors also enables sponsors to take action, where necessary, to remove barriers to the enrollment of representative populations.
10. Sync team calendars to prevent scheduling conflicts.
With limited staffing and a lot of patient visits to manage, calendar visibility helps keep workflows moving and timelines on track.
- Make sure every team member syncs their work calendars.
- Choose a setting that allows all team members to view each other’s available time slots, so visits can be assigned quickly and without double-booking.
Digital features like connected calendars enable teams to boost clinical research collaboration, particularly across visit management.
11. Digitize patient visit checklists to ensure workflow continuity.
Attach a digital visit checklist to each patient profile in your database. The checklist should reflect protocol needs, from I/E criteria to procedures. During each patient visit, the team member working with the patient can check off each task that is specific to that visit. As a result:
- Team members can easily hand off visits as needed, since each staff member can see exactly what needs to get done and record the completion of that task.
- Staff members can save time on unnecessary conversations, since everything they need to know for the visit is right there in the checklist.
- No steps in the protocol are missed.
Easy win: Clinical trial scheduling software features like digital checklists can improve team collaboration while reducing the risk of protocol deviations.
12. Send visit reminders to patients to keep the enrollment timeline on track.
People have a lot on their mind – especially patients who may be juggling medications and other appointments on top of a disruptive medical condition. Send a quick and simple text, phone call, or email reminder about their upcoming site visit to ensure that patient does not miss their time slot, while saving the time it would take to reschedule. Consider sending a notification one or two days in advance of the visit, and include:
- The date of the visit
- The time of the visit
- The address for the visit
13. Set up visit reminders for site staff to keep the enrollment timeline on track.
Site staff have a lot on their mind, too, whether it is the details of a complex protocol or a long list of patients to manage. Set up an automatic email reminder a day before or on the day of a patient visit to ensure that patient gets the care they need, while keeping your workflow on track.
- When setting up your calendar with a patient visit, look for a “reminder” option and choose a helpful date and time.
- Take this same step when you are assigning other team members to a visit.
14. Take the time to fully educate your patients about the trial to support retention.
Don’t risk getting a patient through the pre-screening process and then losing them to a perceived burden or concern. As part of the informed consent process, your team is already required to provide information about the study’s purpose, treatment details, and possible discomforts and risks. But make sure to also have a conversation early on about:
- Any doubts or concerns the patient has about participation.
- Any details that can help reduce the patient’s sense of burden.
- The steps in the screening process.
Whether you can help motivate them, provide additional information, or refer them to the PI with any follow-up questions, you can help the patient feel confident and comfortable about their choice to enroll.
/breast-cancer-clinical-trial_compressed.webp?width=741&height=410&name=breast-cancer-clinical-trial_compressed.webp)
15. Discuss the benefits of the trial with patients, to motivate their participation.
Many patients are hesitant to participate in trials, and may even be distrustful of them. Talk about what participating in the study means to them. Perhaps they have a sense of purpose in contributing to a study that can benefit more people after them. Or maybe this trial feels like their last hope in responding to a treatment. Learn their reason, so they can remember their “why.”
- Consider adding a note about this to their patient file, so various team members can support this patient, too.
16. Set up automated processes around clinical trial billing.
Manual processes around billing can cause two main issues. They can be time-consuming, which increases workload and detracts from patient-focused activities. They can also lead to inaccurate invoicing, which can limit a research site’s income and affect the ability to take on additional studies.
Make financial management easier by using software to automate processes around clinical trial billing, tracking, and budgeting. For example, choose a system that automates tracking of invoiceable activities. Not only can this empower you to build accurate invoices, but this can clear more time for patient care and protocol adherence.
17. Notify sponsors of obvious obstacles early, so they can take actionable steps to support your site.
Keep a digital record of pre-screening data across your patient database to identify problem areas early on during recruitment and enrollment. Here are a few red flags to look out for:
- Low numbers of patient referrals.
- Patterns in I/E criteria failures during pre-screening.
- Patterns in I/E criteria failures during screening.
- Imbalances in demographic representation.
Reach out to your sponsor contact if you do notice any of these recurring issues. When a sponsor knows about recruitment and enrollment inefficiencies early in a clinical trial through secure data sharing, they can intervene with protocol amendments, referral partner campaigns, or other methods of support for your site. This helps keep enrollment timelines on track.
Sites: Ready to kick off clinical trial enrollment workflow optimization?
Check off the 17 steps above and you’re on your way to better collaboration, better workflow efficiency, and an increase in enrollment numbers. Get patients access to the therapies they need, sooner. Also looking for an easy-to-use enrollment performance management platform with valuable reporting features and visit management capabilities already built in to help you complete the 17 steps above? Learn more about StudyTeam for Sites.
Related Posts

How Does a Trial Manager in Greece Improve Clinical Trial Operations with StudyTeam®?
Dimitris Tziogas, local trial manager at a biotechnology company in ...
Read More
How to Address Key Clinical Trial Challenges, According to Clinresco Centres in South Africa
There’s no single solution to overcoming a research site’s specific ...
Read More
3 Clinical Trial Billing Challenges Research Sites Solve with StudyTeam
Challenge 1: Complicated coverage analysis Challenge 2: Tedious budgeting ...
Read More


.png?width=64&name=OST%20Transparent%20(1).png)